One of the testable areas in cardiac pathology is the time course of myocardial infarction morphology. Students can be expected to correlate the gross and microscopic changes with the patient’s clinical timeline.
Here’s the cleanest breakdown.
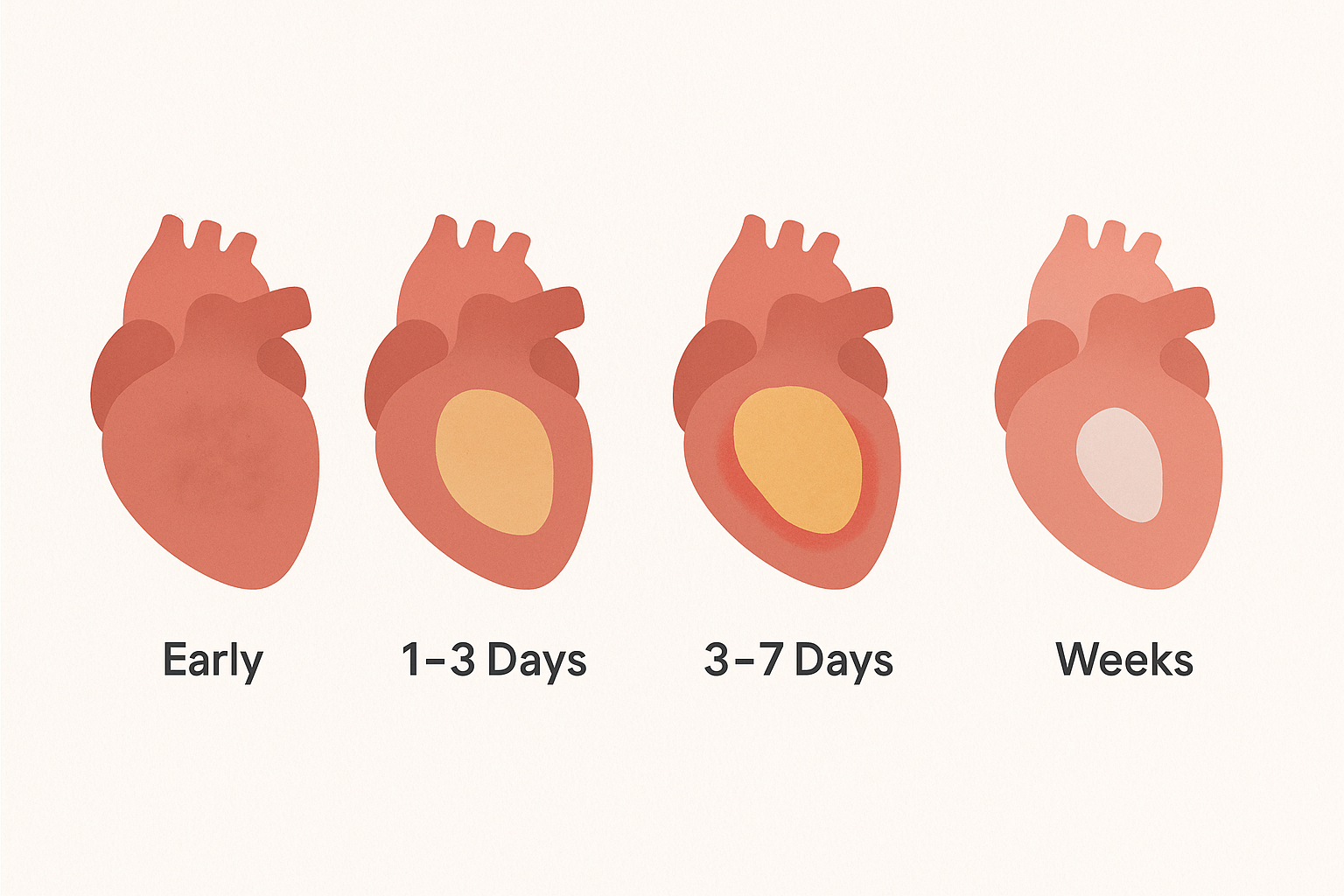
0–4 Hours
Gross Features: None
Micro: Usually none, however variable wavy fibers at the borders are sometimes seen
Clinical: Sudden death from arrhythmia is possible
4–12 Hours
Gross Features: Occasional dark mottling
Micro: Early coagulative necrosis, edema, hemorrhage
12–24 Hours
Gross Features: Dark mottling
Micro: Neutrophils begin to arrive, coagulative necrosis, hypereosinophilia, pyknosis of nuclei, contraction band necrosis
1–3 Days
Gross Features: Mottled yellow-tan center
Micro: Peak neutrophilic infiltrate, coagulative necrosis with loss of nuclei and striations
3–7 Days
Gross Features: Hyperemic border; central yellow-tan softening
Micro: Macrophages begin to remove dead tissue, dying neutrophils
Risk: Ventricular wall rupture is highest here. This is when lysis of necrotic myocardium is maximal and when much of the infarct has been converted to soft, friable granulation tissue
7–10 Days
Gross Features: Maximally yellow-tan and soft, with depressed red-tan margins (healing is just starting)
Micro: Well-developed phagocytosis of necrotic tissue, granulation tissue begins forming at the margins
10–14 Days
Gross Features: Depressed red-gray infarct borders (healing underway)
Micro: Well-established granulation tissue with new blood vessels and collagen deposition
2–8 Weeks
Gross Features: Gray-white scar, progressing from border toward core of infarct
Micro: Increased collagen deposition
>2 Months
Gross Features: Scarring complete
Micro: Mature fibrosis/dense collagenous scar
High-Yield Exam Tips (What the Boards Love to Ask)
🕒 <12 Hours
- Gross changes may be absent
- “Wavy fibers” = early microscopic finding at the border zone; not always present
- Sudden death from arrhythmia may occur before any gross or micro changes appear
🕒 1–3 Days
- Peak neutrophils
- Yellow-tan center begins to appear
- Loss of nuclei/striations = coagulative necrosis
🕒 3–7 Days
- Highest risk of ventricular free wall rupture (boards test this)
- Macrophages break down dead tissue → myocardium becomes soft and friable
- Red hyperemic borders are often present
🕒 7–14 Days
- Granulation tissue
- Fibroblasts + new vessels → healing phase
- Borders appear red-gray
🕒 Weeks to Months
- Gray-white scar → collagen deposition
- Dense fibrosis replaces myocardium → substrate for arrhythmias
- “Scar tissue” questions usually imply >2 months post-MI
This table alone is worth memorizing for the ASCP boards.